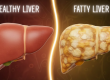
Panic: a very strong feeling of fear and anxiety that causes a person to act without thinking normally.
Given that cholesterol and fats are cited as primary causes of heart disease – and heart disease is the number one cause of death in the world – there is a massive amount of panic surrounding cholesterol and fats.
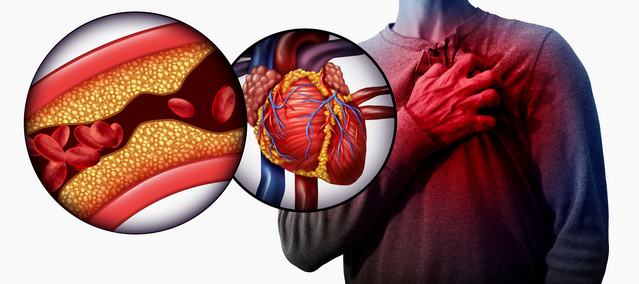 Heart disease is on the rise.
Heart disease is on the rise.
In the confusion, we clearly hear:
1) Bad cholesterol
2) Good cholesterol
These are fictional terms.
There is no such thing as “bad” or “good” cholesterol. Cholesterol is cholesterol.
Cholesterol is associated with various heart diseases, arterial blockages, heart attacks, and strokes. If all that panic were based on facts, it would mean that all people with these conditions have high cholesterol. But that is not the case.
The Truth About Cholesterol
Risks are easily mentioned, but it is not so easily mentioned how essential cholesterol is for life.
The body produces cholesterol in much larger quantities than we consume through diet. The membrane of every cell in the body contains cholesterol as its main ingredient. The membrane protects the cell and regulates what can enter it and in what quantity.
Many important hormones are derived from cholesterol – for example, testosterone and estrogen. Without cholesterol, there is no vitamin D production in the body. Bile acids (substances produced by the liver that aid in the digestion and absorption of fats) are obtained from cholesterol. And one more small thing: cholesterol is a key ingredient for creating new cells.
There is no bad cholesterol. (There is only panic.)
When people talk about “good” and “bad” cholesterol, they are actually talking about something else entirely. “Good” and “bad” are outdated but still popular labels that lead to misconceptions. The misconception is partly “bought” and partly stems from obsolete knowledge. On another occasion, we will explain how and why it was bought.
Cholesterol is a fatty substance and does not mix well with water or blood. Therefore, it binds to another substance so it can travel through the blood to the cells and organs that need it.
The Transporters
![Yellowish spheres are lipoproteins | TLECOATL ZYANYA [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)] Yellowish spheres are lipoproteins](https://upload.wikimedia.org/wikipedia/commons/9/90/Dislipidemias1.jpg) The transporters that carry cholesterol are lipoproteins.
The transporters that carry cholesterol are lipoproteins.
These are compounds made of fats and proteins. (Lipos is the Greek word for fat.)
Lipoproteins are also the carriers for other substances, such as vitamins A, D, E, K, and fats.
There are five types of lipoproteins, but the ones most commonly heard of are low-density lipoprotein (LDL) and high-density lipoprotein (HDL).
When people say “bad cholesterol,” they mean LDL, and by “good cholesterol,” they mean HDL.
The truth is that LDL and HDL are not types of cholesterol – they are merely the transporters. The cargo they carry – cholesterol – is the same.
The Difference Between HDL and LDL
HDL – The “Good” Cholesterol
HDL particles are produced in the liver and intestines. They contain more protein than other lipoproteins. This makes them denser, which is why they are called “high-density.”
It is considered “good” cholesterol because HDL collects all the cholesterol that isn’t used by the body and returns it to the liver, where it will be broken down for further use or partially excreted. It possesses protective and anti-inflammatory properties that regulate the immune system.
However, excessively high levels of HDL can also pose a risk.
What functions does the notorious Low-Density Lipoprotein (LDL) perform?
LDL particles carry cholesterol to the cells.
The body cannot function without LDL. Calling it “bad” is tendentious.
![Cholesterol | Arterial plaque | Thickening of arteries | Narrowing of arteries | Manu5 [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)] Cholesterol | Arterial plaque | Thickening of arteries | Narrowing of arteries](https://upload.wikimedia.org/wikipedia/commons/f/f0/Atheroma.jpg) The downside is that LDL particles travel more slowly and can, under certain conditions, get stuck in the bloodstream. Once stuck, they begin to break down in reaction with other particles. When broken down, LDL particles can, under certain conditions, much more easily penetrate the arterial walls. This creates plaque (buildup in the arteries), hardening and narrowing them. This is one of the ways heart health deteriorates.
The downside is that LDL particles travel more slowly and can, under certain conditions, get stuck in the bloodstream. Once stuck, they begin to break down in reaction with other particles. When broken down, LDL particles can, under certain conditions, much more easily penetrate the arterial walls. This creates plaque (buildup in the arteries), hardening and narrowing them. This is one of the ways heart health deteriorates.
It logically follows that the more LDL particles there are in the body, the higher the chances of cardiovascular (heart and blood vessel) diseases. This is very different from “how much total cholesterol the LDL particles are carrying.”
However, this does not mean that small LDL particles are bad or unnecessary. They are essential for delivering nutrients to places where large LDL particles cannot reach. In any case, LDL is essential for life. Essential, not bad.
Necessary Parameters
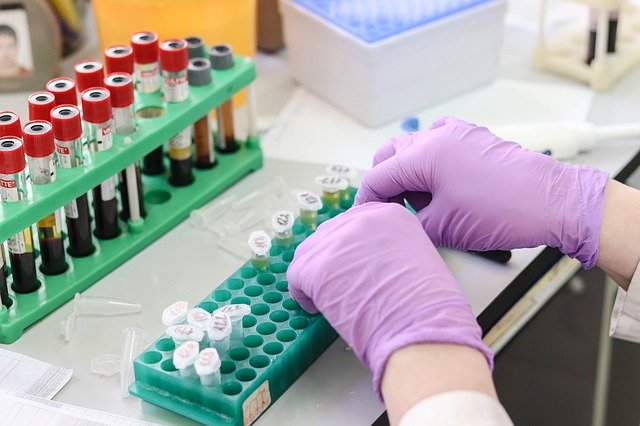 Standard blood tests do not measure the number of LDL particles, nor their size (which is also important), but rather the total amount of cholesterol present in the LDL and HDL particles. From the time such tests were state-of-the-art until now, many new findings have been established and many old ones debunked. But some think that once you finish your studies, there’s nothing more to learn.
Standard blood tests do not measure the number of LDL particles, nor their size (which is also important), but rather the total amount of cholesterol present in the LDL and HDL particles. From the time such tests were state-of-the-art until now, many new findings have been established and many old ones debunked. But some think that once you finish your studies, there’s nothing more to learn.
This means a standard test doesn’t distinguish how many “transporters” exist. It only shows the weight of their total cargo. Meanwhile, what matters is the number of transporters and their size or cargo capacity. The more numerous and smaller the LDL particles are, the easier it is, under certain conditions, for them to penetrate the arteries and form deposits or blockages. This can happen even if the total LDL is within normal limits.
Therefore, it is not true that an elevated level of LDL in the blood automatically represents a risk. It might be, but it might not. Similarly, a normal level of LDL doesn’t mean there is zero risk. Other parameters are needed to determine actual risk. A “risk” determined by a standard test is, at best, a limited assumption for many reasons:
- One reason is that a low level of HDL has the same effect as a high level of LDL, even if LDL is within normal limits. This is because HDL is the cleaner of unused LDL.
- Another essentially important reason is the size of the transporter, i.e., the LDL particle.
- There are other factors, also of essential importance, that determine whether even a small LDL particle will enter the arterial wall. For example, factors contributing to its interaction with certain types of particles in the body, which increases the tendency of the LDL particle to penetrate the wall.
- The smaller the LDL particles, the higher the chance – under certain conditions – that they will penetrate the arterial wall. Thus, a test showing an elevated LDL level might be interpreted as a health hazard, but if those LDL particles are mainly large, the risk of hardening, narrowing, or clogging the arteries is almost non-existent. This is especially true if HDL is in good concentration and if the fats called triglycerides are within normal ranges.
Triglycerides
Just as amino acids (the building blocks of proteins) are the structural units of protein, fatty acids are the building blocks of fats.
Triglycerides are fat particles. Body fat and all dietary fats – good or bad – contain triglycerides. These are groups of fatty acids joined together, and each “group” contains three fatty acid molecules.
Elevated levels of triglycerides in the blood can increase the risk of heart disease. This does not mean they are bad in and of themselves.
Triglycerides are necessary for storing and utilizing energy.
![Yellowish spheres are lipoproteins | TLECOATL ZYANYA [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)] Yellowish spheres are lipoproteins carrying cholesterol and fats](https://upload.wikimedia.org/wikipedia/commons/9/90/Dislipidemias1.jpg) How do triglycerides travel through the body? They are packed with lipoproteins. One type of these lipoproteins is called VLDL (very low-density lipoproteins). VLDL particles contain triglycerides and cholesterol. After the VLDL particles unload the triglycerides in various parts of the body, the remnants are reabsorbed by the liver. There, they are converted into LDL particles and launched into the bloodstream.
How do triglycerides travel through the body? They are packed with lipoproteins. One type of these lipoproteins is called VLDL (very low-density lipoproteins). VLDL particles contain triglycerides and cholesterol. After the VLDL particles unload the triglycerides in various parts of the body, the remnants are reabsorbed by the liver. There, they are converted into LDL particles and launched into the bloodstream.
Fatty tissues and excess body fat are actually composed of triglycerides (and cholesterol).
Fatty tissues in the body consist of triglycerides, but these fats do not come exclusively from dietary fat. They are created in the liver from excess carbohydrates in the diet. They can also be created from excessive protein intake combined with insufficient fat intake. The ratio of proteins, fats, and carbohydrates in the diet is very important. (Dietary fats alone do not trigger fat storage.)
Carbohydrates are converted into blood sugar. Sugar that isn’t used is stored, and if the storage is already full (which is the case for most people), it is converted into fats (triglycerides) that travel through the blood to be stored as fatty tissue.
A predominantly carbohydrate-based diet, especially if it is within the range of popularly recommended amounts – 45-65% of total calorie intake (the true source of the panic) – enormously increases the chances of elevated triglyceride levels in the blood.
Constant carbohydrate intake – meaning high blood sugar levels – prevents the use of fat for energy (burning triglycerides). If you eat mostly carbohydrates as an energy source, the body will create fat and deposit it.
Why can’t fats be used?
The body doesn’t get a chance to use them because there is always an intake of carbohydrates and thus a need for their conversion into fat.
Insulin must prioritize getting to work to remove excess sugar from the blood (high sugar levels are toxic to the body). Burning fat becomes “irrelevant” because the alarm is set to remove the sugar. Not only does elevated insulin block fat burning, it is also what causes the formation of triglycerides from excess sugars.
Diet and Exercise
In a state of ketosis (a metabolic state where the body burns fat for fuel instead of carbohydrates), HDL levels increase, triglyceride levels decrease (because they become the body’s main energy source and are utilized), LDL particles become larger, and their number decreases, while the total LDL amount may decrease or stay the same. During the adaptation period to ketosis, LDL might even be above the limit because weight loss melts fat from fat cells, releasing the cholesterol stored within them into the blood. Ketosis keeps insulin at a normal, rather than elevated, level; thus, there is no high sugar intake, inflammation, or plaque generation. Furthermore, it activates the hormone glucagon and growth hormone, which are among the primary fat burners.

Minimal amount of carbohydrates
If you change your diet to minimal carbohydrate intake, moderate protein, and high fat, you will switch the body into fat-burning mode. It will begin effectively burning triglycerides instead of accumulating them. There is a specific way of eating to switch the body to fat burning.
 High-intensity exercise, combined with this way of eating, makes the body function on fat burning – burning off excess body fat and dietary fats. This significantly speeds up muscle building. (It does not mean that someone without excess body fat will continue to lose weight.)
High-intensity exercise, combined with this way of eating, makes the body function on fat burning – burning off excess body fat and dietary fats. This significantly speeds up muscle building. (It does not mean that someone without excess body fat will continue to lose weight.)
This combination brings many benefits if practiced correctly, along with the necessary intake of vitamins and minerals, vegetables, water, and sufficient sleep.
Here are just a few of them:

- Better (cardiovascular) health.
- Optimized hormonal system.
- Faster growth of lean muscle mass.
- Faster reduction of excess body fat.
- Simultaneous muscle building and fat loss.
- Increased physical and mental energy.
- Increased mental clarity.
- Better sleep.
- A stronger body.
This is the opposite of the general trend, isn’t it?
Dino Nikolic
Creator and author of Muskultura
Health Coach
Fitness Instructor and Strength and Conditioning Coach
Certified Nutritionist
February 20, 2020
Discover more from Muskultura.mk
Subscribe to get the latest posts sent to your email.